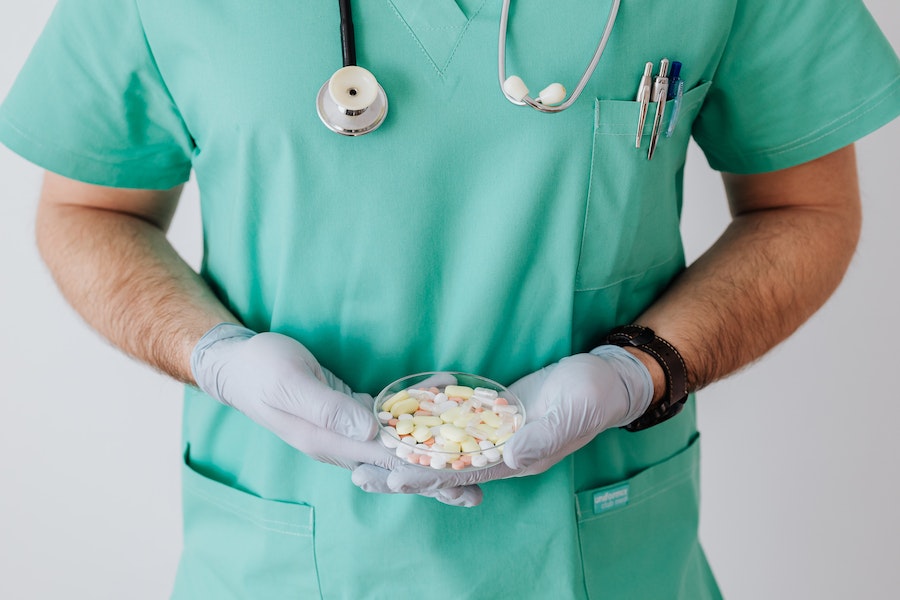
Cyber Security in the Healthcare Industry: Protecting Patient Data
September 22, 2023, 8 min read
What makes healthcare cyber security so crucial? Biotech, insurance, healthcare, pharmaceutical, and medical device businesses, and anybody else involved in the healthcare industry, must prioritize healthcare cyber security as a top business priority. It includes a variety of measures to protect against cyber threats from within and without, to keep patient information private, to keep medical systems and equipment running smoothly, and to keep patient data secure.
Today’s businesses cannot survive without properly implementing information security and cyber security measures. The following are examples of hospital information systems used by many different healthcare organizations:
- Medical prescriptions written and filled using the Internet
- Systems for maintaining medical records digitally
- Helping Hands for Medical Office Management
- Computerized imaging and physics records
- Decision-making aids in the clinic
- Electronic health records (EHRs)
The Unique Challenges of Healthcare Cyber Security
1. Using Stronger Authentication Methods in Healthcare cyber security
There’s no denying that requiring two factors of authentication instead of one improves the safety of your accounts and infrastructure. This extra step in the verification procedure will add a little bit of time, but the total could be longer than you’d think. Other difficulties with MFA in healthcare include using biometrics for authentication while wearing personal safety gear (PPE) or imposing MFA on legacy systems that may not support it.
There are a few viable healthcare cybersecurity solutions that can help with biometrics authentication problems. On iOS, you can use an Apple watch to unlock, while Android users can try out Smart Lock. For legacy systems that do not enable MFA, however, there are limited options. Yet, by partitioning your network, you can lessen your exposure to danger. With VLANs and ACLs, you may partition off the infected hosts and lower the attack surface (ACLs). You should also include computers without MFA in your upgrade schedule and put pressure on the manufacturers to release new software and operating system versions (even though an upgrade may take a very time – at least it helps inform your management of the risks).
2. Should I Install the Patch?
Installing updates regularly is a fundamental practice in cyber security. cyber security in the healthcare sector, however, is more complex. Specialized healthcare equipment might cost hundreds of thousands of dollars or even millions. This hardware can only be used with certain operating systems and has been optimized for certain platforms. When it comes to IT, the lifecycle of the equipment rarely coincides with that of the operating system, which forces businesses to keep supporting antiquated software. It is possible that installing an essential OS patch will cause the manufacturer to stop supporting the device or perhaps void the warranty. The resulting issues may have far-reaching consequences for patient treatment. Due to manufacturer mandates to preserve obsolete software versions, it is not uncommon to observe Windows 7 or even XP still in use when performing penetration tests on hospital networks.
3. Finding a Solution
Unless someone compels manufacturers to upgrade the versions of software and operating systems they support, or unless networks segment individual systems, these holes will persist. Given the scarcity of effective countermeasures, organizations should consider proactive monthly threat hunting as a means to apprehend intruders before they can steal sensitive information or cause irreparable harm.
Thirdly, a difficulty that has been increasing is the hardness of the host. NIST Special Publication 800-123: Guide to General Server Security recommends disabling unused services, programs, and network protocols as part of host hardening.
Strong authentication and suitable resource constraints should also be set up. Few equipment manufacturers back efforts to harden healthcare cyber security systems or devices. If you make any modifications to your system’s settings that diverge from the vendor’s “recommended” configuration, the vendor may cease providing support for your system. Your company spent several million dollars on a radiological device a few years ago, and now the manufacturer refuses to provide maintenance because you disabled unused services, turned on the Windows firewall, or removed local administrator access. One of my most notable pen tests involved medical equipment lacking proper protection. As a result, I gained root access through an exposed online interface using simple administrator credentials.
Again, the solution is to put pressure on the vendor to provide new versions of their supported software and operating systems and to implement network segmentation and access control lists (ACLs) to reduce the attack surface of vulnerable devices. Proactively seeking threats once a month is also recommended.
4. Putting Segmentation into Practice
Segmenting a network, or dividing it up into smaller networks, can be a powerful compensatory control. However, there are drawbacks to segmentation, such as increased workload for IT and networking personnel and more difficult troubleshooting. As a result of these obstacles, healthcare networks are frequently considerably “flatter” than they should be, with devices able to communicate with one another even when there is no compelling financial justification for doing so. Lack of network segmentation makes it easier for malicious software like ransomware to spread throughout the system.
The solution is to have top-level executives discuss network segmentation and come up with a shared strategy for moving forward. There should be strict regulations on segmentation, but striking the correct balance might be difficult.
5. Not enough workers to go around
It’s reasonable to wonder if IT personnel problems are unique to the healthcare sector. Indeed, you would be correct. There are several reasons why healthcare cyber security is particularly vulnerable to this threat. The first reason is that the healthcare industry is “mission-critical,” meaning any downtime is intolerable as it could lead to the loss of human lives. Second, healthcare firms need larger and more capable technical teams than those in most other industries. More devices per user means healthcare IT departments must provide more resources for endpoint support, networking, and security. HIPAA compliance standards are an additional cost for the healthcare industry.
Understanding the Value of Patient Data
Although historical data should not be used exclusively to make treatment decisions, it can be used to create more complete patient profiles. Information on the patient’s prior actions and routines, for instance, could shed light on the cause of the present symptoms. Better health outcomes and happier patients are possible results.
Providers may better communicate with their patients, allocate resources, and ensure that everyone has equal access to care when they combine historical data with newer records. To help providers make sense of their data and get reliable, timely, and actionable insights, a variety of solutions are available.
Consequences of Healthcare Data Breaches
In healthcare, data breaches risk financial harm to institutions and patients. After a cyber attack, facilities must swiftly respond by eliminating threats, patching vulnerabilities, and restoring reputation.
Any of these things might be very expensive to do. Current estimates place the average cost of a data breach at $211 per compromised record, not including the possibility of regulatory fines. These costs should be passed on to your patients, as they come at the expense of research and treatment.
HIPAA and Other Healthcare Cyber Security Regulations
In 1996, HIPAA was enacted to take strong measures against cybercrime in the healthcare sector. Most of the signatures on it can be found on US soil. HIPAA’s primary objective is to prevent unauthorized parties, such as hackers, from gaining access to protected health information stored on healthcare providers’ servers.
Only authorized individuals who fall under HIPAA’s “covered entities” can see or make changes to a patient’s protected health information (PHI).
Selected users submit requests and justifications for server access, which are then verified by HIPAA. If the users don’t meet the criteria, they are immediately prevented from accessing the servers. Currently, HIPAA’s services are only available within the United States, but the organization has plans to grow.
Cyber Security Risks and Threats in Healthcare
Cyber threats can compromise an organization’s ability to deliver essential patient care. The Center for Internet Security, Chief Security Officer, Healthcare IT News, and TechRepublic cite diverse actors for these risks. Healthcare deals with six main breach types: Phishing, malware, ransomware, patient data theft, insider threats, and compromised IoT devices.
Protecting Medical Devices from Cyber Attacks
- Locate and keep tabs on all networked healthcare equipment.
- Classify internet-enabled healthcare equipment.
- Make sure to update the software frequently.
- Create a framework for handling cyber incidents and a plan to respond to them.
Healthcare facilities, including hospitals, are prime targets due to data significance and network scale. Your medical practice can avert hacker attention by avoiding Internet-connected medical devices. Prepare against evolving cyber threats with real-time device monitoring, risk segmentation, software updates, and an effective incident response plan.
The Importance of Employee Training and Education
A lack of cyber security harms healthcare patients even with the preventive provided by the cyber security training required to be HIPAA-compliant.
In 2018, there was a 1,000% increase in healthcare data breaches. If that doesn’t make you sit up and evaluate your healthcare cyber security training program, perhaps these numbers will:
- There was a one-hundred-percent rise in security breaches affecting 884,360 people across 24 separate breaches at health plans. Seventy-five percent of the businesses involved are healthcare providers.
- The first five months of 2018 saw 12 breaches affecting 100,602 customers at small enterprises.
- About three million people were impacted by a security breach before the first half of 2018 was over.
Strategies for Incident Response and Disaster Recovery in Healthcare
Covered companies subject to HIPAA must create an incident response strategy by the Security Incident Procedures standard. Covered companies must develop data backup, disaster recovery, and emergency mode operation plans. However, not all incident response plans are equal, and relying solely on a paper plan might not suffice during a security breach. Healthcare institutions need tailored incident response plans that suit their unique requirements.
Since healthcare businesses must act swiftly to contain cyber security events without also disrupting excellent patient care, they are particularly at risk. Because of this, stopping and responding to cyber threats swiftly can be challenging.
The Role of Cyber Insurance in Healthcare Cyber Security
Data breaches, theft, system hacking, paying ransomware extortion, and other forms of cybercrime can all result in significant financial losses for enterprises. Your small business needs cyber insurance if it keeps private data online or in electronic form.
Future Trends and Technologies in Healthcare Cyber Security
Experts in the field of cyber security have identified many noteworthy trends:
- Authentication with several methods
- Solutions for Biometric and Secure Access at the Service Edge (SASE)
- The development of the CIO has created a centralized authority for data protection.
- Managed and hosted services continue to grow
- The Expansion of Zero-Trust Security
Conclusion
As a result, healthcare organizations must prioritize cybersecurity to safeguard patient information and operational infrastructure. Implementing access controls, keeping tabs on network activity, performing frequent vulnerability assessments and penetration tests, and having an incident response strategy in place are all crucial to securing the healthcare industry. Healthcare providers can better safeguard patient information and prevent system compromise by adhering to these recommended procedures.